Heel Pad Syndrome
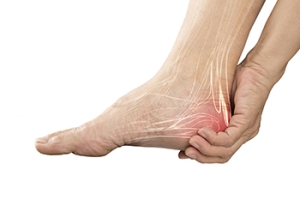
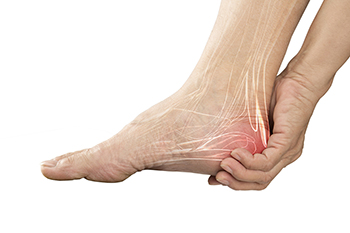 Heel pad syndrome is a painful condition affecting the heel's fatty tissue, leading to discomfort and difficulty walking. This syndrome occurs when the heel's fat pad, which acts as a shock absorber, deteriorates or thins out, often due to excessive stress or injury. The condition can result from aging, repetitive high-impact activities like running or jumping, prolonged standing, or being overweight. Heel pad syndrome can affect anyone but is more common among athletes, older adults, and individuals with occupations requiring extended periods of time on their feet. Symptoms typically include a deep, bruised feeling in the heel, particularly noticeable during weight-bearing activities. This pain can be sharp or aching, worsening with activity and improving with rest. If you have painful heels, it is suggested that you schedule an appointment with a podiatrist who may prescribe orthotics, heel cups, specific exercises, and anti-inflammatory medication.
Heel pad syndrome is a painful condition affecting the heel's fatty tissue, leading to discomfort and difficulty walking. This syndrome occurs when the heel's fat pad, which acts as a shock absorber, deteriorates or thins out, often due to excessive stress or injury. The condition can result from aging, repetitive high-impact activities like running or jumping, prolonged standing, or being overweight. Heel pad syndrome can affect anyone but is more common among athletes, older adults, and individuals with occupations requiring extended periods of time on their feet. Symptoms typically include a deep, bruised feeling in the heel, particularly noticeable during weight-bearing activities. This pain can be sharp or aching, worsening with activity and improving with rest. If you have painful heels, it is suggested that you schedule an appointment with a podiatrist who may prescribe orthotics, heel cups, specific exercises, and anti-inflammatory medication.
Many people suffer from bouts of heel pain. For more information, contact one of our podiatrists of Ankle & Foot Care Center. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Jupiter, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
Definition and Relief Methods of Morton’s Neuroma
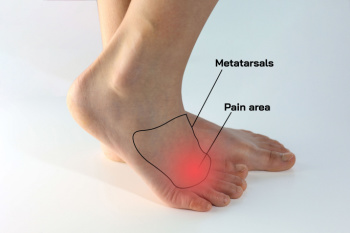
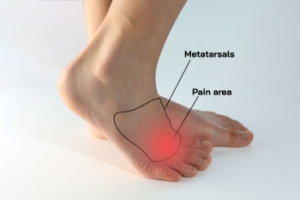
Morton's neuroma is a compressive neuropathy of the forefoot interdigital nerve, that results in a thickening of tissue surrounding the nerves leading to the toes. It typically affects the nerves between the third and fourth toes. This condition causes pain, numbness, or a burning sensation in the ball of the foot, often worsened by wearing narrow shoes or high heels that squeeze the toes together. Relief methods focus on alleviating pressure on the affected nerve, such as wearing shoes with a wide toe box to reduce compression. Padded inserts or orthotics can help to distribute weight evenly and support the arch, relieving strain on the forefoot. Massaging the area can reduce inflammation and provide temporary relief. In severe cases, corticosteroid injections or surgical removal of the neuroma may be considered to alleviate persistent symptoms and restore comfort and function to the foot. If you have pain in this part of your foot, it is suggested that you promptly schedule an appointment with a podiatrist who can successfully diagnose and treat Morton’s neuroma.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact one of our podiatrists of Ankle & Foot Care Center. Our doctors will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Jupiter, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What is Morton's Neuroma?
Morton’s neuroma, (also referred to as Morton’s metatarsalgia, Morton’s neuralgia, plantar neuroma or intermetatarsal neuroma) is a condition that is caused when the tissue around one of the nerves between your toes begins to thicken. This thickening can result in pain in the ball of the foot. Fortunately, the condition itself is not cancerous.
Morton’s neuroma affects women more often than men with a ratio of 4:1. It tends to target women between the age of 50 and 60, but it can occur in people of all ages. There are some risk factors that may put you at a slightly higher risk of developing the condition. People who often wear narrow or high-heeled shoes are often found to be linked to Morton’s neuroma. Additionally, activities such as running or jogging can put an enormous amount of pressure on the ligament and cause the nerve to thicken.
There usually aren’t any outward symptoms of this condition. A person who has Morton’s neuroma may feel as if they are standing on a pebble in their shoe. They may also feel a tingling or numbness in the toes as well as a burning pain in the ball of their foot that may radiate to their toes.
In order to properly diagnose you, the doctor will press on your foot to feel for a mass or tender spot. He may also do a series of tests such as x-rays, an ultrasound, or an MRI. X-rays are usually done to rule out any other causes for your foot pain such as a stress fracture. Ultrasounds are used to reveal soft tissue abnormalities that may exist, such as neuromas. Your podiatrist may want to use an MRI in order to visualize your soft tissues.
There are three main options for treatment of Morton’s neuroma: Injections, decompression surgery, and removal of the nerve. Injections of steroids into the painful area have been proven to help those with Morton’s neuroma. Decompression surgery has been shown to relieve pressure on the affected nerve by cutting nearby structures such as the ligaments in the foot. Another treatment option would be to surgically remove the growth to provide pain relief.
If you suspect that you have Morton’s neuroma you should make an appointment with your podiatrist right away. You shouldn’t ignore any foot pain that lasts longer than a few days, especially if the pain does not improve.
Why Live with Pain and Numbness in Your Feet?
Symptoms and Risk Factors for Toenail Fungus
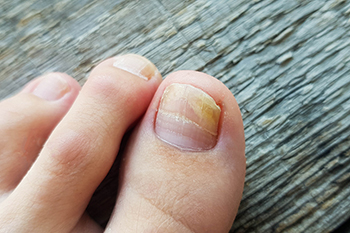
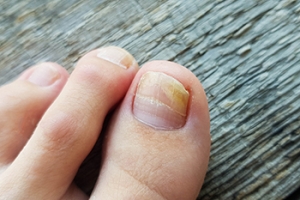
Toenail fungus, also known as onychomycosis, is a fungal infection affecting the toenails. It typically begins as a white or yellow spot under the tip of the nail and can spread deeper into the nail over time, causing discoloration, thickening, and crumbling of the nail edges. Risk factors for toenail fungus include frequent exposure to warm and moist environments such as public showers, wearing tight-fitting shoes, and having a weakened immune system. Symptoms may include a foul odor from the infected nail, pain or discomfort, and difficulty trimming the nail due to its thickness. If left untreated, toenail fungus can lead to permanent damage to the nail bed and spread to other nails or skin. The chances of recovery increase when treated early. If you have toenail fungus, it is suggested that you contact a podiatrist where you can receive expert treatment for this condition.
For more information about treatment, contact one of our podiatrists of Ankle & Foot Care Center. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in Jupiter, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Toenail Fungus
Toenail fungus is a frustrating problem that affects many people. It can be persistent and hard to get rid of. As many different types of fungi are present throughout the environment, it is very easy to contract toenail fungus.
The feet are especially susceptible to toenail fungus because shoes and socks create the ideal dark and moist environment that fungal infections thrive in. While fungal infections of the nail plate are quite common, if left untreated they can spread beyond the toenail and into the skin and other parts of the body.
Signs of toenail fungus include a thickened nail that has become yellow or brown in color, a foul smell, and debris beneath the nail. The toe may become painful due to the pressure of a thicker nail or the buildup of debris.
Treatment for toenail fungus is most effective during the early stages of an infection. If there is an accumulation of debris beneath the nail plate, an ingrown nail or a more serious infection can occur. While each treatment varies between patients, your podiatrist may prescribe you oral medications, topical liquids and creams, or laser therapy. To determine the best treatment process for you, be sure to visit your podiatrist at the first signs of toenail fungus.
Understanding and Managing Plantar Fasciitis
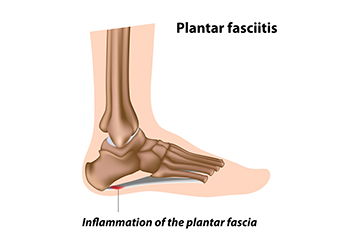
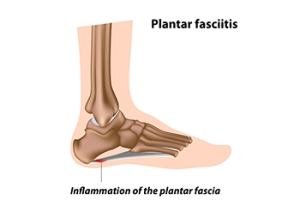
Plantar fasciitis is an inflammation of the plantar fascia, the thick band of tissue along the bottom of the foot, connecting the heel to the toes. Symptoms can include sharp heel pain, especially with the first steps in the morning or after long periods of rest. Diagnosis is typically based on a physical examination and patient history, sometimes supplemented by imaging tests. Relief tactics involve a combination of rest, stretching exercises, and proper footwear with good arch support. For persistent cases, orthotic devices or medical interventions such as corticosteroid injections may be necessary. Early and consistent treatment is key to alleviating symptoms of plantar fasciitis and preventing chronic discomfort. If you have heel pain, it is strongly suggested that you promptly contact a podiatrist who can accurately diagnose the problem, and treat it accordingly.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact one of our podiatrists from Ankle & Foot Care Center. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our office located in Jupiter, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Definition and Types of Corns
Corns are thickened areas of skin that develop due to repeated friction or pressure, often on the feet. They typically form on the tops or sides of toes and can be painful when pressed. There are two main types of corns which are hard and soft. Hard corns are the most common, appearing as small, dense, and circular areas of thickened skin, usually found on the tops of toes or other bony areas. Soft corns, in contrast, are whitish and rubbery in texture, typically developing between the toes where the skin is moist from sweat. Both types of corns result from excessive pressure and friction, often due to wearing ill-fitting shoes or abnormal toe movements. Corns on the feet can be painful and may cause difficulty in completing daily tasks. If you have developed a corn, it is suggested that you speak to a podiatrist who can offer you effective relief options.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact one of our podiatrists of Ankle & Foot Care Center. Our doctors will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
- Wearing properly fitting shoes that have been measured by a professional
- Wearing shoes that are not sharply pointed or have high heels
- Wearing only shoes that offer support
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Jupiter, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.